|
Due to the complex nature of these injuries, surgical management remains a challenge for the attending surgeon. In this article, the authors conducted a comprehensive literature review on the epidemiology of sacral fractures, relevant anatomy of the sacral and pelvic region, common sacral injuries and fractures, classification systems of sacral fractures, and current management strategies. Depending on the fracture location, neurological injury may be present in over 50% of cases. Few large-scale studies have addressed postoperative complications or long-term results, but current evidence suggests that although fusion rates are high, long-term morbidity, such as residual pain and neurological deficits, persists for many patients.ĪB - Sacral fractures are uncommon lesions and most often the result of high-energy trauma. 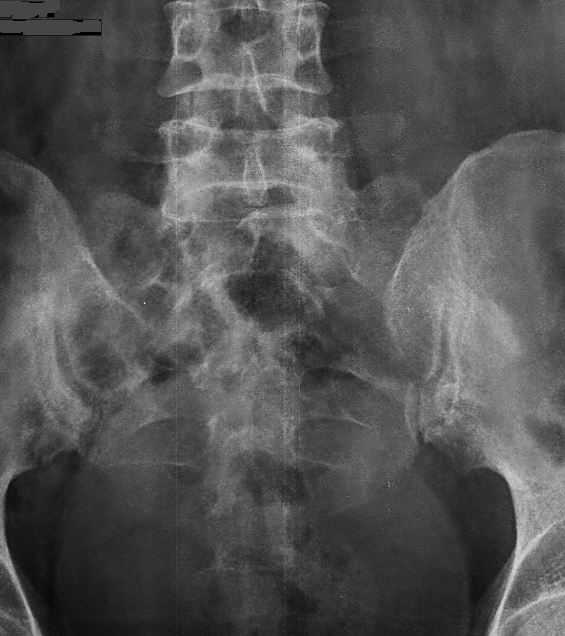
It should remembered that pelvic fractures usually heal within 6-8 weeks, but that primarily ligamentous injuries may need longer protection (3-4 months).įracture healing and pelvic alignment are monitored by regular X-rays every 4-6 weeks until healing is complete.N2 - Sacral fractures are uncommon lesions and most often the result of high-energy trauma. Significant weight bearing is usually possible by 6 week but use of crutches may need to be continued for three months. Progressive weight bearing can begin according to anticipated healing. Assistance with leg lifting in transfers may be necessary. In unstable unilateral pelvic injuries, weight bearing on the injured side should be limited to "touch down" (weight of leg). Generally, the patient can start to sit the first day after surgery and begin passive and active assisted exercises.įor unilateral injuries, gait training with a walking frame or crutches can begin as soon as the patient is able to stand with limited weight bearing on the unstable side. Mobilization can usually begin the day after surgery unless significant instability is present. Upper extremity and bed mobility exercises should begin as soon as possible, with protection against pelvic loading as necessary. This must be communicated to physical therapy and nursing staff.įor all patients, proper respiratory physiotherapy can help to prevent pulmonary complications and is highly recommended. It is important that the surgeon decide how much mechanical loading is appropriate for each patient's pelvic ring fixation. The following guidelines regarding physiotherapy must be adapted to the individual patient and injury. Anterior arch fixation increases stability.Spinopelvic fixation (especially for comminuted transforaminal vertical sacral fractures).1 or 2 additional screws (S1 or S2 level).Fixation can be enhanced by one or more of the following: A washer is advisable for secure fixation on the ipsilateral side.įixation failure may occur, especially with grossly unstable injuries. 
However, a screw that maintains excessive distraction increases the risk of nonunion. Thus, a fully threaded (position) screw may be preferable to a lag screw for ISS fixation. ISS for sacral fractures can be unilateral, extending far into the contralateral sacral ala, transsacral, or transiliac extending beyond the contralateral ilium where a suitable nut on the screw threads can enhance fixation.Ĭompression of a comminuted alar fracture may injure a nerve root within the fracture zone. Screw channels for sacral fractures are narrow and precise screw placement is therefore essential. 
ISSs for sacral alar fractures are usually oriented transversely because this is the path of a transsacral channel.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
